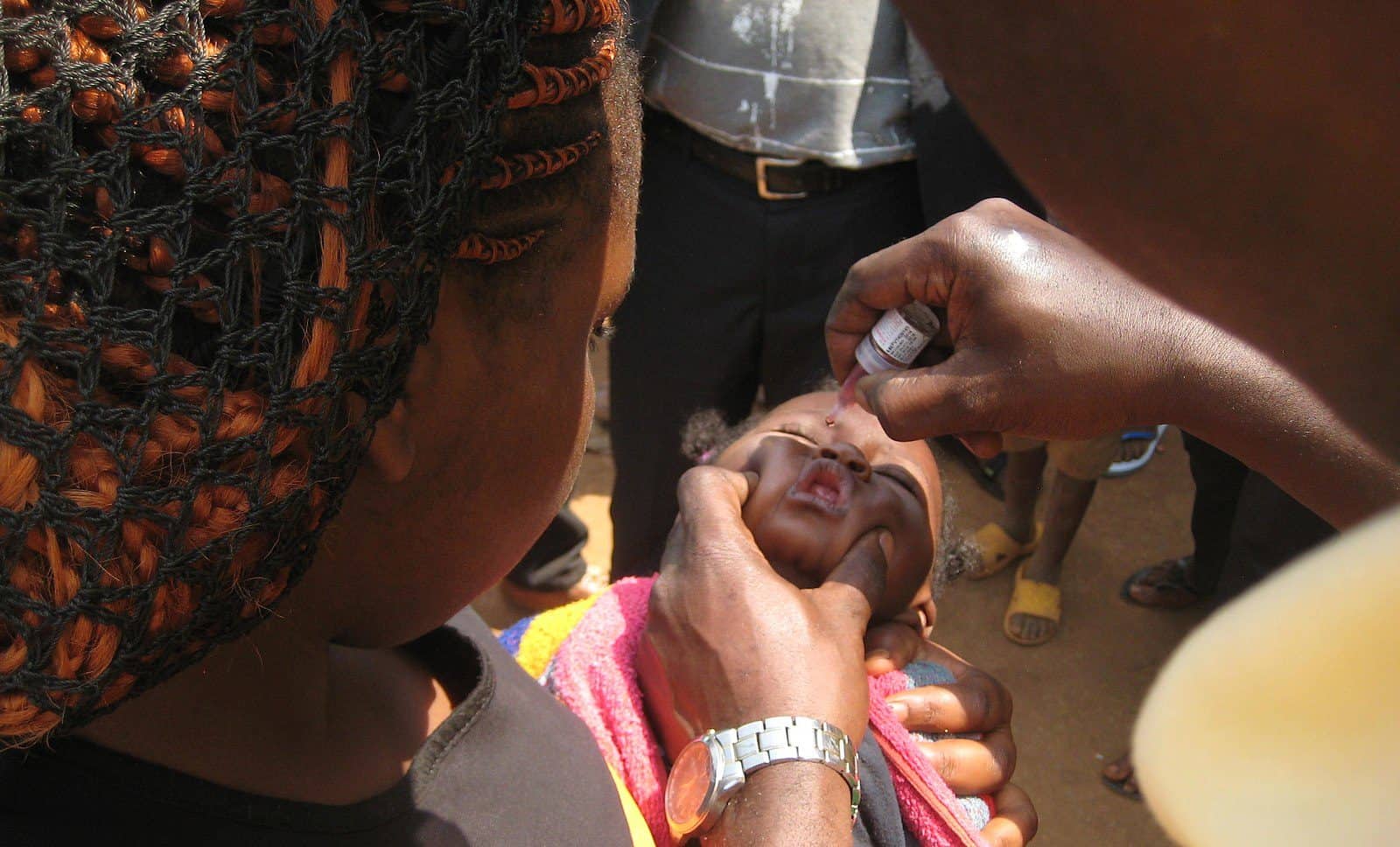
A young child receives oral polio vaccine dose. Photo credit: Louie Rosencrans/CDC. Licence: CC-BY-2.0
Estimated reading time: 5 minutes
Despite massive progresses in the last decades, infectious diseases remain a major threat to young children’s life and health in low- and middle-income countries. This burden affects children unequally, with the most disadvantaged most at risk. As the pandemic threatens the global progress towards the Sustainable Development Goals, what can be done to ensure a fair and healthy start in life?
by Elodie Besnier
Millions of children are beginning their lives at a disadvantage
The COVID-19 pandemic has brought infectious diseases back at the forefront of Europe’s health concerns. Yet, these diseases have remained a major threat to health globally long before the latest pandemic, especially for young children. In 2019 in low- and middle-income countries (LMICs), more than two million children under five years old – the equivalent of Paris’ entire population – died from common infectious diseases.(1) This burden disproportionally falls on the most disadvantaged groups. For example, in over thirty LMICs, children in the poorest households are more than twice more likely to die before their fifth birthday than their wealthier counterpart. Urban children tend to have a better chance of survival and better access to health services than their rural counterparts. Yet, inequalities also exist within these populations, with the most disadvantaged urban children sometimes faring worse than their rural counterparts.(2)
These inequalities result from the determinants of health. Health is determined by both biology and where and how you live. Unlike your genes, these are elements you, your community or society as a whole influence, which in return, will affect health in your family, community or even globally. Young children are particularly vulnerable to such inequalities as they are so dependent on others for all their needs. Yet, these first few years of life are fundamental for child development and for the health of the adults they will become, or even the health of their future children. Addressing child health inequalities help prevent the tragedy of a child’s death or illness. It also supports a healthy future for your community and society as a whole.
Reviewing the evidence of public health interventions in LMIC
The world has committed to end preventable child deaths and reduce inequalities by 2030 with the Sustainable Development Goals. We therefore need strong evidence to guide interventions that can not only improves child health at the national level, but also reduce these inequalities to give every child an equal chance. Bringing together researchers from the Norwegian University of Science and Technology (NTNU), Newcastle University and Durham University, the Centre for Global Health Inequalities Research (CHAIN) reviewed evidence from public health interventions in seventy-two LMICs and their effect on child health and inequalities due to infectious diseases.(3)
Can we achieve a double-win for child health?
Some interventions can not only improve child health at the population level but also reduce certain inequalities by improving the health of the most disadvantaged children. This mainly consists in interventions aiming to increase the demand and use of preventive tools like vaccine or bed-nets, and includes education activities with communities and caregivers, information campaigns or social mobilization and outreach.

However, this double-win effect is not systematic. Interventions that are beneficial to one type of disadvantaged group may not have the same benefit for another. For example, service integration (bringing various child health services in the same facility) can be improve immunization coverage at population level and in urban populations . However, it can also increase inequalities between rural and urban children. At the opposite, zinc supplementation can help reduce pneumonia in children living in slums or low-income neighbourhood but its benefit for a wider group of children is less clear.
Finally, large gaps remain as to the health inequality effect of entire fields of public health interventions. For example, it is broadly unknown how using legal, regulatory, or enforcement mechanisms to safeguard public health can help address the burden of infectious diseases equitably.
Filling the research gap to give all children a healthy, more equitable start in life
Policy makers and societies in the Global South need strong, reliable scientific evidence about what works and the children it works for. On the road to a more equitable start in life lie three challenges for research.
A lack of research from or in the Global South
The first comes from the comparative lack of health inequalities research from or in the Global South. Context-specific research must respond to the context-dependent nature of health inequalities. For example, the evidence behind interventions targeting HIV-exposed infants or the adoption of selected new vaccines only comes from a handful of countries. The evidence supporting selected water, sanitation, and hygiene (WASH) interventions or nutrition supplementation – although promising – is still insufficient to lead to solid global recommendations. Hence, we need more attention (and support) from the research community on the issue of health inequalities in the Global South. At the same time, primary studies and reviews carried out in LMICs should report on health inequalities dimensions more systematically.
The quality of health inequalities research is mixed
A second challenge is the quality of current health inequalities research, which also hampers decision and policy making. Current research quality standards may still need to be further promoted. However further efforts should also be dedicated to developing capacities, knowledge, and methodologies suited to research in LMICs.
Health equity is a political choice
Finally, the ultimate challenge to a more equitable start in life remains political, not only in the way health inequalities research is used, but also in the way a society defines success and the criteria for it. Researchers may help answer the question “what works” and “who for”. Society and communities alone can answer “who do we care about”.
References
- Global Burden of Disease Collaborative Network. Global Burden of Disease Study 2019 (GBD 2019) Results [Internet]. Seattle, United States: Institute for Health Metrics and Evaluation (IHME); 2020. Available from: http://ghdx.healthdata.org/gbd-results-tool
- UNICEF. Advantage or Paradox? The Challenge for Children and Young People of Growing Up Urban [Internet]. UNICEF; 2018 Oct p. 38. Available from: https://www.unicef.org/publications/index_103399.html#
- Besnier E, Thomson K, Stonkute D, Mohammad T, Akhter N, Todd A, et al. Which public health interventions are effective in reducing morbidity, mortality and health inequalities from infectious diseases amongst children in low- and middle-income countries (LMICs): An umbrella review. PLOS ONE. 2021 Jun 10;16(6):e0251905. https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0251905

Elodie Besnier
Elodie Besnier is a PhD candidate at the department of Sociology and Political Science at the Norwegian University of Science and Technology (NTNU) in Trondheim, Norway. Her research at the Centre for Global Health Inequalities Research (CHAIN) focuses primarily on health interventionsimpactinghealth inequalities in children in low- and middle-income countries.